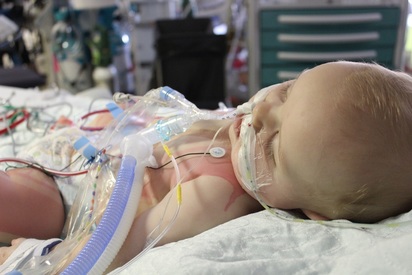
As you can imagine, the last couple days have been pretty intense. We've had some pretty scary lows but are now starting to look up. So, without further ado, here is a look at the last few days: the surgery and first 24 hours.

The night leading up to surgery was uneventful. Baby slept really well, ate when he was supposed to and didn't ask for more when I couldn't give it to him. Of course neither Chris nor I slept very well but James had no idea what was coming so he slept blissfully through the night, just like we had hoped. It was another early start though since we slated as the first surgery of the day. At 5am our alarm went off, we got ready for the day, then woke up James just long enough to get him changed and ready to go.
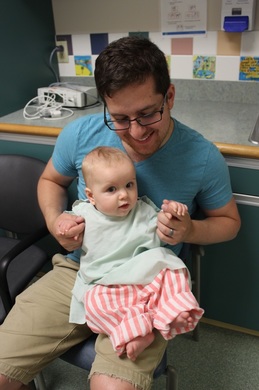
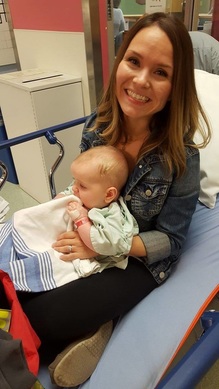
I got to hold James while we rode on his stretcher up to the pre-op room, past the 30-somethings and elderly heart op patients to a room in the corner for baby's/kids that had a window into the nurses station and some toys and books to play with before going into the OR. Of course James was a hit with all the nurses, because who doesn't love a cute baby who's all smiles and giggles because he's oblivious to what's about to happen? Dr. Ross and our anesthesiologists came by to say good morning before heading into the room and once they were ready I was suited up to bring James into the OR.

I carried him down the hall and into the OR where I help him as they gave him the gas before putting in the IV. Once my job was done I made my way back to the pre-op room to get Chris and then headed up to that oh so familiar fishtank to wait. It was now 7:45 and were told to expect the surgeon around noon. I settled in and updated the family while Chris went to grab us some breakfast, and then it was our turn to distract ourselves for a change.

The Wait
Waiting is always the hardest part. You're so on edge and want to help but there's nothing you can do. The surgery itself is to repair his RVOTO or right ventricle outflow tract obstruction via pulmonary artery augmentation. I wish I knew the medical terms for this procedure but it seems like this time around we had less information provided to us and really had to encourage nurses and doctors to give us more specific information beyond "this medication will make him sleepy". I totally understand why they do that, but it's so frustrating when I want to know what is happening and I don't get that information. So you just ask, throw out some more medical terms while they explain it in layman's terms, and then hope to get something more specific. Sometimes it works, sometimes it doesn't.
Finally, at 11:45am, 15 minutes ahead of schedule, Dr. Ross came down the hall with his report.
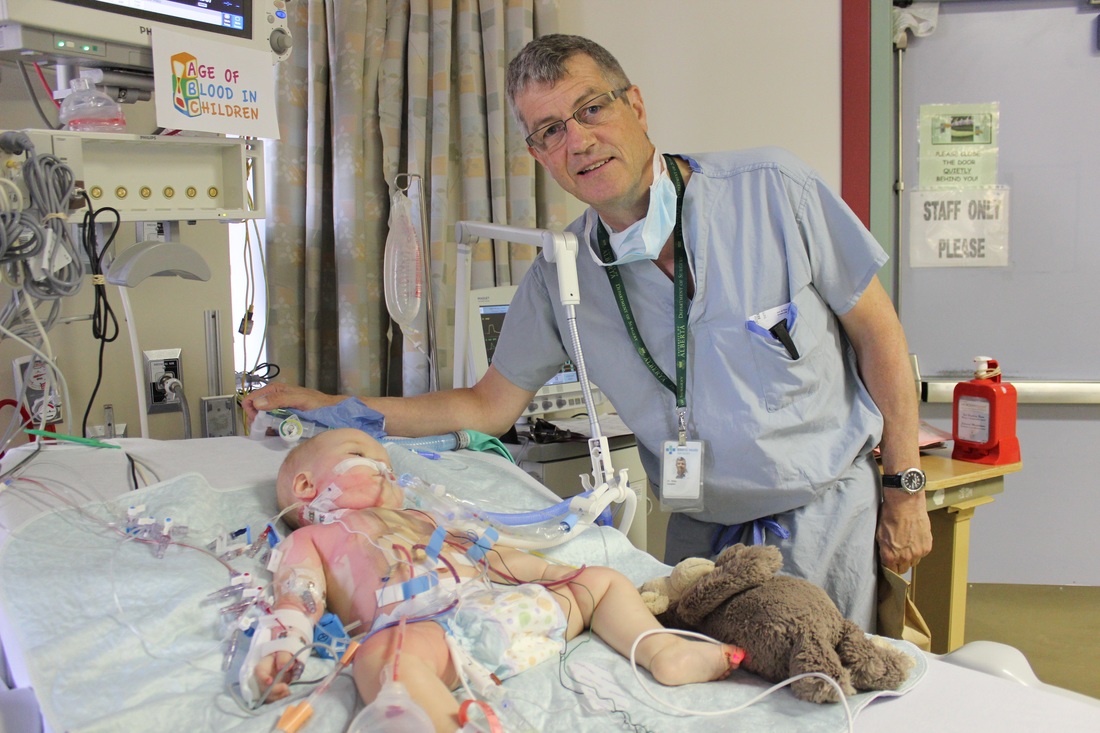
Results
The surgery was MOSTLY successful. They were able to augment the main part of the pulmonary artery enough to greatly alleviate the pressure. However there is still a gradient narrowing in the left branch (the part that is twisted) that is ok for now but may require another balloon valvuloplasty in a few years. They were also able to save the pulmonary valve itself but it came at a cost. There is a gradient narrow just above the valve but if they had augmented the artery any closer to the valve it would have been destroyed. So for now they'll monitor it and hopefully it will not require replacement until he's an adult. And while the surgery did alleviate the primary issue, it did leave behind mild leaking from the pulmonary valve. Honestly, at this point his heart sounds like a washing machine with all murmurs caused from the leaking tricuspid valve, pulmonary valve, and residual VSD, but, it works.
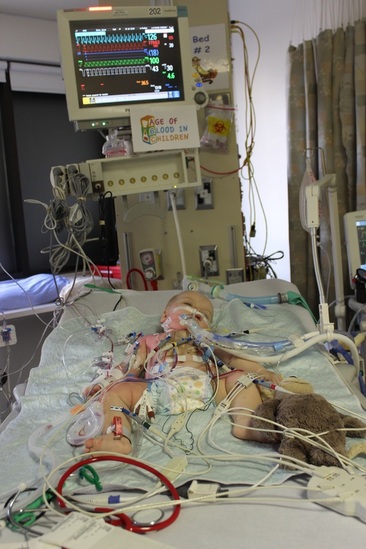
But of course the first wasn't over yet. As we had learned from James first open heart surgery, the first 24 hours are the most critical for survival. And while we'd spoken we the surgeon we still had to wait another hour for him to come out from the anesthetics.
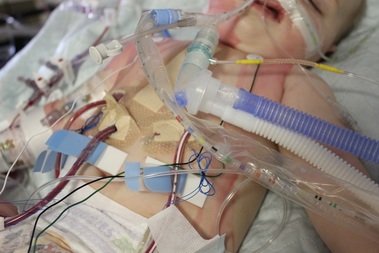
The First 24 Hours
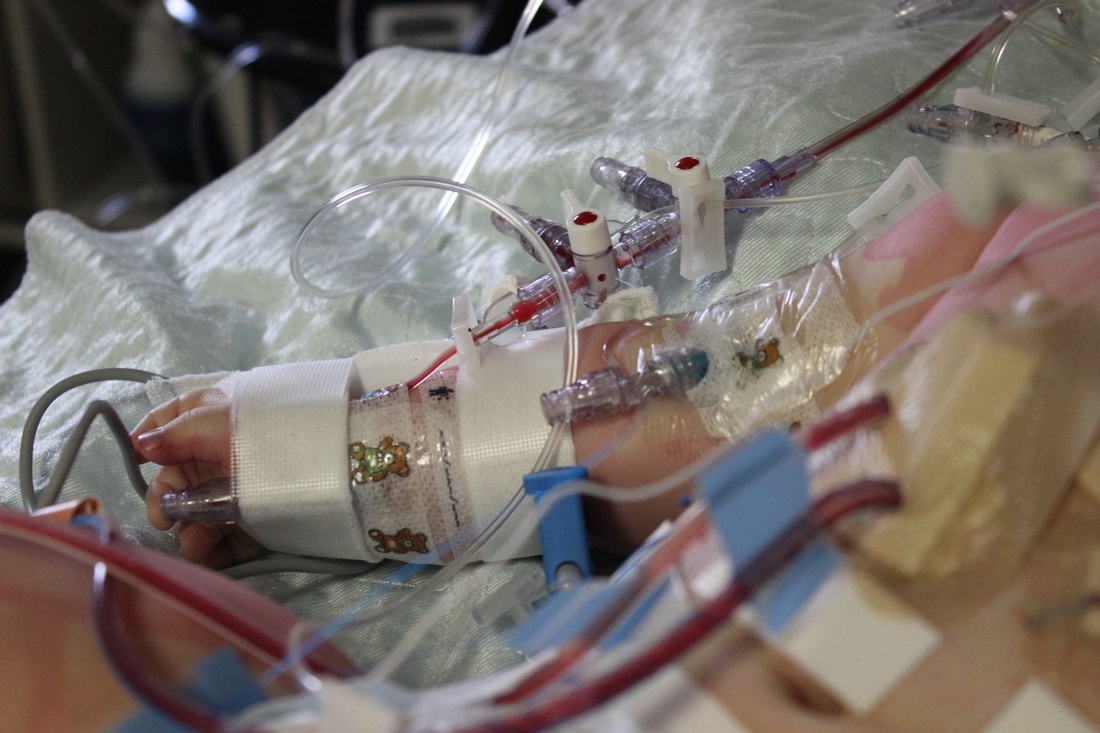
As we started to approach the one hour mark I began to pace the hall in the hopes of catching a glimpse of James as he was transfers from the OR to the PCICU (pediatric cardiac intensive care unit). Just as I was going to sit back down I saw his bed out of the corner of my eye! I rushed over and waved at Chris to come with me and we got to see our little monkey. He was lucky in that his heart hadn't healed to the breast plate as we had feared, so the bypass machine was able to be hooked up normally rather than through the femoral artery. Of course we didn't get to follow him just yet, so after thanking our surgeons, nurses, and anesthetic team we went back to wait again until the nurses in the PCICU were able to switch over all his lines and get him hooked up to the monitors in their unit.
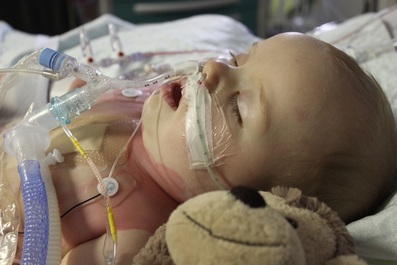
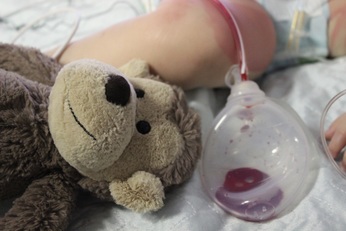
Don't Forget To Breathe
James' vitals were looking good and he seemed to be recovering well, so only a couple hours on the unit and we'd already been told he'd likely be able to have the ventilator turned off and have him extubated later that afternoon! Last time this didn't happen until day 2 so we were thrilled to cut that time down to less than a day! They began the process of slowly trying to get him off the machine before taking out the tube, and of course we had to wait until he woke up too. A couple hours later... and he was still riding the machine and hadn't woken up. We waited, and waited... We were starting to worry when the unit doctors were coming around and asking why he still hadn't woken up and that he should have been up over an hour ago. Finally, he started to twitch. He was still on morphine so he was pretty out of it, but he was starting to come around. They called over the RT and got ready to extubate. The respiratory therapist was really fantastic and let us stick around for the extubation right at bedside.
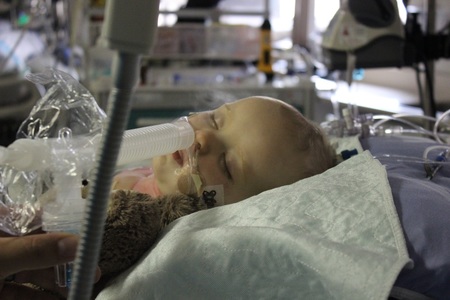
And with that the RT turned off the ventilator and removed the tube. We watched... and he wasn't breathing. At all. Not even trying to breath. He just lay there, completely still with the colour draining from his body. As his lips began to turn blue Chris grabbed my hand. Our nurse and the RT, cool and calm as ever, started to prop him up, shook him, gave him a jaw thrust to try and open his airway and held the high flow to his face. Still nothing. Not even a sign of struggle. Just completely limp. More RT's started to show up and doctors joined our bedside. We had probably 10 people around our bed. After over 2 and a half minutes of absolutely no breathing (which, for the record, felt like an eternity) he started to struggle! He wasn't breathing, but he was trying to gasp.This continued for 20 minutes where his oxygen saturation was peaking around 38% with no sign of any sort of regular breathing pattern establishing itself.They kept trying to wake him up more and finally got him going with a nebulized epinephrine. It was basically an epi-pen but vaporized. His heart rate was through the room (over 200bpm!) but he was breathing. It was shallow and laboured, but he was breathing. After sitting with him another 20 minutes Chris and I decided to run back to our hotel room to grab a quick bite to eat before heading back to the hospital. We didn't want to leave until he seemed settled so we took this as our opportunity to get away really quickly.
The break was just what we needed. Mentally and physically we were drained and exhausted. That quick moment to just sit down and clear our heads really helped. And after our dinner we headed back to the hospital.
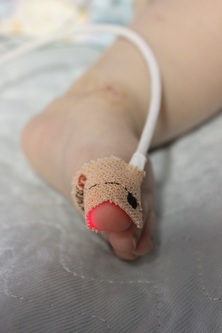
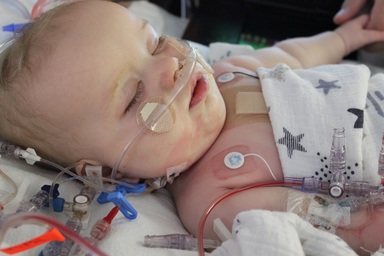
We'd only been gone 45 minutes but when we arrived we saw the RT's around our bed again, and James was struggling to breath... We asked them how long it had been going on and they said about 30 minutes. They were giving him more of the nebulized epinephrine and applying the jaw thrust but his throat had swollen from the tube removal and wasn't allowing air to pass through. His breath was so shallow and sounded like a high pitched hiccup as he struggled to get in air. A third dose of the epinephrine was administered... and then a 4th. The RN who was holding the "gun", or "smoking barrel" as Chris likes to call it, had be exposed to so much epinephrin that she was shaking!
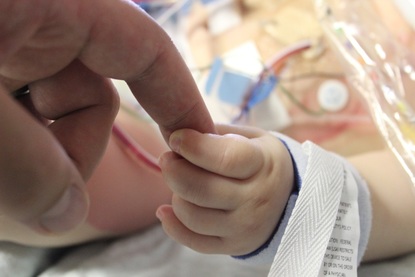
Apparently what had triggered the breathing episode was his bolus of morphine. It wasn't a large dose by any means, but morphine is a respiratory suppressant, and as we discovered, James is extremely sensitive to narcotics. This was one of those "OOOOOOHHHH! THAT"S why" moments for me and Chris. It totally explained why he had such violent withdrawal from morphine the first time around! And probably why he struggled with sleep apnea in the NICU where they loved to give him a bolus of morphine any time he didn't want to settle down. It all makes sense now. So while we were planning on having "the drug talk" with him anyway (we're somewhat responsible parents), we now know we'll want to have that talk a lot sooner and really let him know that narcotics are just not an option for him if he really insists on being an idiot at some point.
Thursday, July 14, 2016
Too Much Of A Good Thing
We woke up early this morning feeling nervous about what the day had to bring. I've been struggling quietly with pain in my breasts this whole time too because I haven't been able to feed baby. I always knew I had an over supply (look at the size of my baby!), that I'm prone to mastitis (I've had it twice), and my supply is super sensitive to oats (two handfuls of honey nut cheerios before bed... and I was engorged within three hours), but I'm super sensitive to pumping! I've noticed that the stimulation ups my milk supply, but the pump doesn't actually get all the milk out. So I'm pumping for 20 minutes, getting combined total of 6-8oz and still engorged every time. It hurts to touch, it hurts to pump, it hurts to do anything. I'm actually scared by the idea of weening because I don't see how I'm going to decrease my supply without getting mastitis again. Anyway, I hadn't slept well because of that and thinking about baby, but I was ready to go.
*As an aside, especially to any of the breastfeeding support group girls, I was able to freeze my milk this time and didn't have to pour it down the drain like last month!
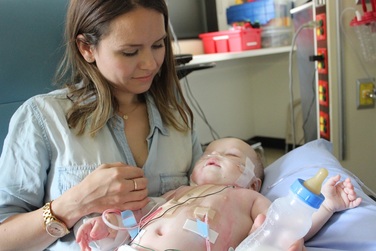
We got to the hospital in time for rounds and were pleasantly surprised to see Brittany at hour bed! She was one of our favourite nurses when we were first in Edmonton, so it was great to catch up with her. Seriously, she's amazing. Anyway, we weren't sure what to expect so we were a little anxious to see how he was doing. Praise God, he was doing SO WELL! It was truly a miracle. From barely breathing and in terrible shape the night before, to this sad, but conscious baby, breathing well on his own... He was doing so well that in rounds he was approved to have his Central Venus Line, medial chest drainage tube, pacing wires, catheter, ART-line, and NJ-tube removed THAT MORNING! AND he was well enough that, provided there was a bed available, James would be moving to the cardiac ward on 4C THAT AFTERNOON! We could hardly believe it! For everyone who got my mom and dad's prayer request yesterday, those prayers were answered! It was like night and day! He was much more alert already and was so much happier, albeit still grumpy, than he was yesterday. So with things looking up, and the promise of moving to the ward this afternoon, Chris headed off to run a secret errand. His staff at St. Boniface Diocesan had given us a gift card for Cookie's by George, and we wanted to share the sweet love by buying a box of cookies as a thank you to the PCICU staff... and of course get a few cookies for ourselves too. lol. The Milk Chocolate Chip is just Ah-Mahzing.
By the time he came back we'd been able to get all those lines removed, leaving only his nasal cannula, heart rate, respiratory rate, SpO2, the two side drainage tubes (wish I could remember what they were called), and one IV. We took turns cuddling our little monkey and before we knew it, it was time to head up to the ward!
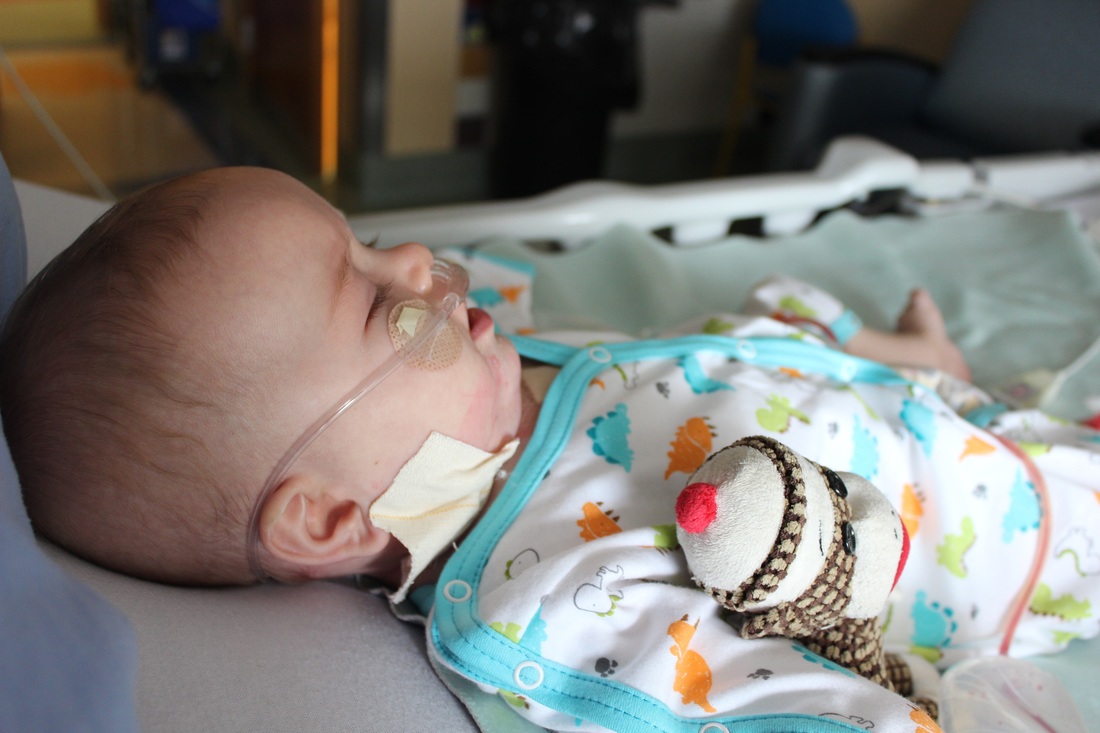
Hospital Couture
Considering how intense the previous day had been, today was a breeze! Once we got him all settled in to his new digs we got to dress him in his new custom hospital gown! Dariel, our little friend Theodore's mum, had told us about this place in Winnipeg called Itty Bitty Baby (click the link to go to their website - you can contact Carol for more ordering options!) that makes clothes for premies, micro-premies, and baby/children's hospital gowns. So before we left we ordered two gowns for James that she made special rush order for us so we'd have them before we left. I don't know why they don't carry these in hospital gift shops! They have the snaps on the sleeves too so it doesn't matter how many lines or wires your little one has, you can still dress them in their own clothes.
A Little Relief
Finally by the end of the day I was given permission to try breast feeding James. Oh my goodness, what a relief it was to me! It helped SO much. But apparently James ate more than he could handle. He'd eaten a lot that morning (15oz in one go!) but then hadn't really eaten since then. But I think he over ate because next thing we knew he was throwing up like crazy. We rolled him into recovery to keep him from choking then called the nurse to help with the clean up. Once we got him settled he went right to sleep so Chris and headed out for dinner.

 RSS Feed
RSS Feed
