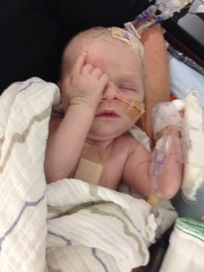
Tuesday, January 12, 2016
It was another day in the NICU. Not much had happened over night and things looked like they were improving again, slowly but surely. His feeds seemed to go well overnight and they had been listening to his chest for signs of congestion, which could indicate chylothorax build up, but hadn't noticed anything concerning. His next chest X-ray to verify this was scheduled for Wednesday morning and in the mean time the medical team had approved him to increase his feeds.
He was now eating regularly, every three hours, and being bumped up 1ml each feed. He was now up to 11ml, but based on his age should now be eating closer to 120ml each feed, so he still had a long way to go. But the lactation consultant was in and had offered to help me throughout the day.
At first, things were a little rough. Because he'd only ever had hard soothers, a soft empty breast was not really doing it for him. So he'd fight and cry and didn't want to latch. I wasn't really worried about it because I'd been warned it's hard to breastfeed NICU babies, but I was surprised that he was struggling since he'd been showing all the signs of wanting to breastfeed for quite a while now. He had really good suction on his soothers, and was always rooting around. I wasn't really sure what I was doing wrong. Fortunately they have one of best lactation consultants around at the Stollery so I knew I was in good hands.
It was another day in the NICU. Not much had happened over night and things looked like they were improving again, slowly but surely. His feeds seemed to go well overnight and they had been listening to his chest for signs of congestion, which could indicate chylothorax build up, but hadn't noticed anything concerning. His next chest X-ray to verify this was scheduled for Wednesday morning and in the mean time the medical team had approved him to increase his feeds.
He was now eating regularly, every three hours, and being bumped up 1ml each feed. He was now up to 11ml, but based on his age should now be eating closer to 120ml each feed, so he still had a long way to go. But the lactation consultant was in and had offered to help me throughout the day.
At first, things were a little rough. Because he'd only ever had hard soothers, a soft empty breast was not really doing it for him. So he'd fight and cry and didn't want to latch. I wasn't really worried about it because I'd been warned it's hard to breastfeed NICU babies, but I was surprised that he was struggling since he'd been showing all the signs of wanting to breastfeed for quite a while now. He had really good suction on his soothers, and was always rooting around. I wasn't really sure what I was doing wrong. Fortunately they have one of best lactation consultants around at the Stollery so I knew I was in good hands.
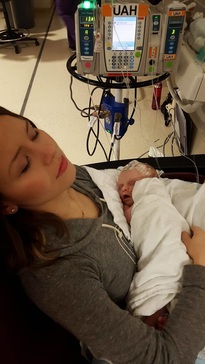
She was so knowledgeable and patient, and really helped me and baby. You could tell she was very passionate about her job helping mums and babes figure things out, since she truly gave you her undivided attention. When cross body hold wasn't working, she had me try football. That was a bit better because we've noticed he really likes to look around, but it still wasn't great. She had me try a nipple shield as a transition tool, helped me with improving my positioning (though she gave me the greatest compliment when she said she was surprised this was my first baby because I seemed to be a natural!), and gave me some tips for when baby really doesn't want to settle. However he was still struggling, and would get really mad when he realized he had to actually work for this. But then, for a moment, he got it. For probably 5 minutes straight he had a good latch and was actively working. After those 5 minutes you could tell he was tired because his breathing was becoming more rapid and eventually he let go of his latch. But it was the best he'd done (third time's a charm I guess!), and she was happy with his progress.
Interestingly enough, she said the reason he was struggling was that he wants instant gratification. He doesn't want to work for his food, he wants it to just be there. So for James in particular she recommended no bottles at all for at least the first 2-3 months. She warned me that some of the nurses would not be thrilled by this since it requires a few extra steps on their part, but that in the long run it would make all the different in the world. I wasn't sure how to let our nurses know about this request without sounding like a crazy high maintenance mum, but she took the heat off for me and put a big notice in his file so that I didn't actually have to say anything; it had come as a medical recommendation.
Each time she worked with us it got easier and easier. He is still fussy at first, but once he gets going it seems to go pretty smoothly. Since getting these feedings going is his last step to going home to NICU Winnipeg, it was definitely something I needed to work on diligently.
Interestingly enough, she said the reason he was struggling was that he wants instant gratification. He doesn't want to work for his food, he wants it to just be there. So for James in particular she recommended no bottles at all for at least the first 2-3 months. She warned me that some of the nurses would not be thrilled by this since it requires a few extra steps on their part, but that in the long run it would make all the different in the world. I wasn't sure how to let our nurses know about this request without sounding like a crazy high maintenance mum, but she took the heat off for me and put a big notice in his file so that I didn't actually have to say anything; it had come as a medical recommendation.
Each time she worked with us it got easier and easier. He is still fussy at first, but once he gets going it seems to go pretty smoothly. Since getting these feedings going is his last step to going home to NICU Winnipeg, it was definitely something I needed to work on diligently.
The Pump Room Girls
Ok, so one of the strangest things I've experienced throughout this whole process has been the pump room. To me, the pump room used to imply a pool shack where I would balance chemicals and prime the pumps while I was lifeguarding wading pools throughout university. But now, the pump room has taken on a whole new meaning. Now, it is a sterile room with 4 pumps where mums can go to pump for their babies. In Winnipeg there was only one pump so you'd have complete privacy to pump by yourself. Here, with so many babies in the unit, all 4 pumps are being used almost all the time.
The first time I entered the room, I didn't know where to look. Here I was, two days postpartum in a room full of women, sitting around with their boobs out (pumping, obviously), and chatting! It was so weird. They had created their own sort of NICU subculture to help cope with the stress. Conversations seemed to flow from comparing milk supply, to how their babies were doing, and other random gossip that seemed to come up. I've never experienced anything like this before, and I was really glad I wasn't super conservative or self-conscious about myself or the whole thing could have been a whole lot more awkward.
After about a week of trying to fit in and add my two cents in the various conversations it seemed I had finally been accepted! One of the mums revealed to me that they had nick-named me "Miss Glorious" when they first met me because apparently no one should look that put together two days postpartum. Of course at the time I had felt like a swollen marshmallow but revealing this did not win me any bonus points with the mums. lol. They told me I looked "shiny". I don't know what that means, but it was pretty hilarious.

Winding Down
That evening on our way back to the hospital, after our dinner and gym session (this is my accountability check in 2 weeks postpartum photo), we bumped into our friends from PCICU from Winnipeg in the hall. We got the update on their little one and gave them the latest on ours. They have been through so much with their little peanut, and the fact that they can remain so positive in the face of it all, even after hitting rock bottom (they have really seen the absolute worst scenarios you could possibly imagine) is so inspiring. I hope to be like them in how I handle stress.
While we were chatting they gave us advice as to what we should take and/or request when we transfer back to Winnipeg, and I had mentioned to them about one mom back home in Winnipeg who had reached out to me. Turns out they knew about her too (she seems to be a bit of a legend out here since their little one had to stay for an entire year!), and talked about possible play dates once everyone was home and well.
Both of these families had also created heart story pages on Facebook to chronicle their journey and keep family and friends updated on what was going on. After reading a bit of both their stories, I was blown away by the peace and grace with which they handled these tough situations. But in addition, I discovered that both of these mums were also Christians and their faith became very evident through their stories. It was like another mini God moment for me, where the family I had connected with the most while here, and the mom that reached out to me at home, both shared my faith as well. It may not mean much to some people, but it has given me a sense of comfort and peace.
And now we continue to wait and see what the next day brings.
And now we continue to wait and see what the next day brings.

 RSS Feed
RSS Feed
